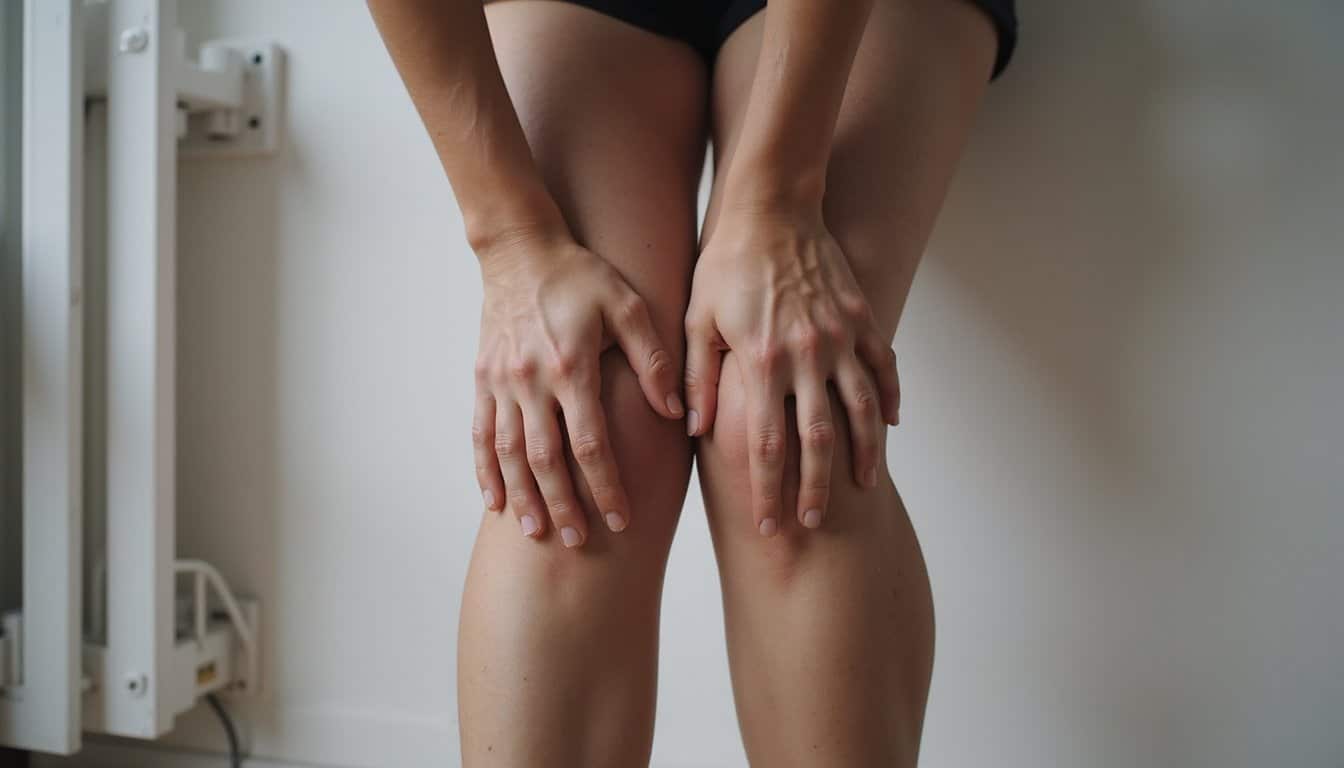
When you see someone in the “fentanyl fold,” you’re witnessing fentanyl’s extreme potency overwhelming their brain’s mu-opioid receptors. The drug’s 50-100 times greater strength than morphine triggers rapid central nervous system depression, shutting down both consciousness and the core muscle tone needed to stay upright. Their spine curves inward while their head drops forward, yet they remain semi-standing. Understanding why fentanyl makes people bend over, and the pharmacology behind this dangerous posture can help you recognize when someone needs immediate intervention.
What Is the Fentanyl Fold?
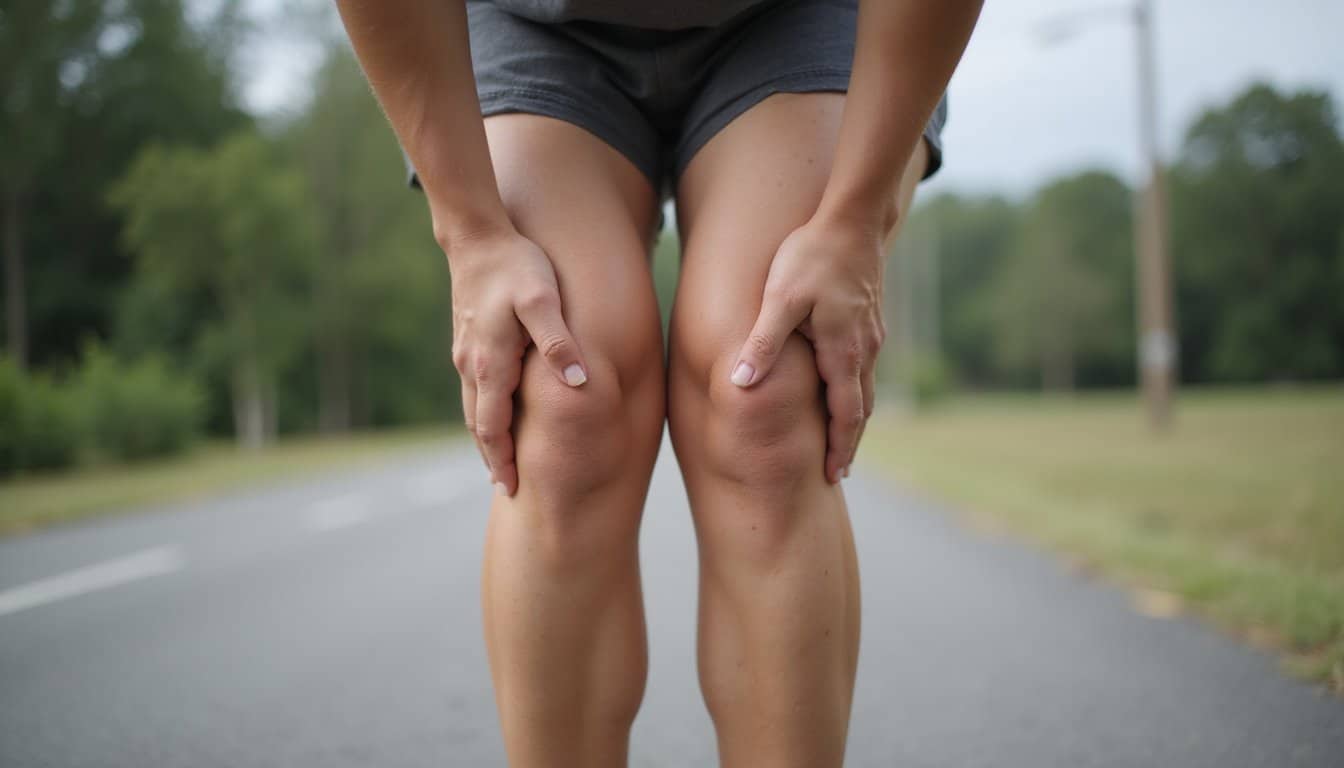
The fentanyl fold refers to a distinctive posture where a person bends sharply at the waist while their head drops forward, yet their body remains semi-upright rather than collapsing completely. You’ll notice the spine curves inward, arms hang limp, and knees stay bent in what resembles a frozen, semi-conscious state. The person typically shows minimal eye movement or a glazed gaze and remains unresponsive to noise or touch. This folding posture can last for minutes or hours, resembling sleep when observed from a distance.
This posture results from opioid muscle relaxation combined with opioid nervous system suppression. When fentanyl binds to receptors in your brain and spinal cord, it triggers CNS depression effects that disrupt normal motor function. You experience loss of postural control because the drug impairs your body’s ability to correct imbalance. Impaired balance opioids cause, paired with opioid motor impairment, prevents you from maintaining an upright position despite remaining partially conscious.
Why Fentanyl Hits the Brain Harder Than Other Opioids
Fentanyl’s extraordinary potency stems from its 75-100 times greater strength compared to morphine and its exceptionally high binding affinity for mu-opioid receptors. This means your brain experiences profound neurological effects at remarkably low doses.
| Factor | Fentanyl | Morphine |
|---|---|---|
| Relative Potency | 75-100x | 1x |
| Receptor Binding | Highest affinity | Standard |
| Brain Oxygen Drop | Up to -65% | Moderate |
| Respiratory Onset | 4 min before sedation | Concurrent |
| Fentanyl Coordination Loss | Severe | Mild-moderate |
Your breathing impairs four minutes before alertness changes, creating dangerous hypoxia while you’re still conscious. Mu-receptor activation occurs at 1,700-times lower concentrations for respiratory effects than sedation, explaining why fentanyl coordination loss and postural collapse happen so rapidly. Research shows that fentanyl-induced oxygen decreases occur not just in the NAc but also in the amygdala, demonstrating that this dangerous hypoxic response affects multiple brain regions simultaneously. This is why there is no safe amount of fentanyl outside of clinical settings where trained specialists can monitor and respond to these life-threatening effects.
How Fentanyl Shuts Down Muscle Control and Consciousness

When fentanyl floods your brain’s opioid receptors, it triggers severe central nervous system depression that impairs both consciousness and muscle coordination within minutes. Your core muscles lose the tone needed to maintain an upright posture, while simultaneously your brain’s alertness centers shut down, preventing you from correcting your balance. This dual effect, muscle weakness combined with diminished awareness, explains why you can’t simply will yourself to stand straight during fentanyl intoxication. The danger intensifies because fentanyl is 50-100 times stronger than morphine, meaning even tiny amounts can overwhelm your body’s ability to function normally. These effects can linger for 45 minutes to an hour or longer, as fentanyl accumulates in fat tissue and takes time to clear from your system.
Brain Function Slows Dramatically
Because fentanyl binds to opioid receptors in the brainstem, the region controlling breathing, heart rate, and consciousness, it systematically shuts down the body’s most critical functions. The opioid physical effects begin with respiratory depression, occurring at drug concentrations 1,700 times lower than those causing sedation. Your breathing slows approximately four minutes before you notice any changes in alertness. fentanyl’s impact on opioid sedation extends beyond immediate physical effects, leading to profound changes in patients’ overall state of consciousness. As tolerance builds, individuals may unknowingly reach for higher doses, increasing the risk of overdose and further complicating their recovery process. Understanding the nuances of fentanyl’s influence is essential for developing effective treatment strategies for those struggling with opioid dependency.
Fentanyl disrupts neurotransmitter release, suppressing substance P and flooding your dopamine system. This manipulation rewires your brain’s reward pathways while impairing cognitive function in the cerebral cortex. You’ll experience compromised decision-making, attention deficits, and memory impairment. These deficits can persist long after discontinuation, significantly impacting daily functioning and quality of life. The drug also triggers intense withdrawal symptoms that drive continued use, creating a devastating cycle of dependence.
The drug produces a distinct EEG signature, indicating profound neurological disruption. As brainstem suppression intensifies, you lose consciousness, but only after respiratory depression has already endangered your life.
Muscles Lose All Tone
The paradox of fentanyl’s effect on muscle tissue lies in its ability to cause both profound relaxation and dangerous rigidity, sometimes simultaneously in different muscle groups. When you’re exposed to high-dose fentanyl, your central nervous system experiences severe opioid-induced weakness, causing postural muscles to lose their ability to keep you upright.
What happens to your muscles:
- Your back and neck muscles collapse, forcing your torso into involuntary forward hunching
- Your diaphragm and intercostal muscles stiffen, losing their normal respiratory rhythm
- Your abdominal muscles enter tonic contracture while limbs flex abnormally
- Your motor neurons receive disrupted signals, creating unpredictable strength loss
This dual mechanism, relaxation in postural muscles combined with rigidity in respiratory muscles, explains why you can’t maintain an upright position while simultaneously struggling to breathe. Research has shown that fentanyl-induced muscle rigidity causes a significant decrease in compliance of the respiratory system, making it even harder for the lungs to expand during breathing attempts. The danger is amplified by the fact that fentanyl is up to 100 times more potent than morphine, meaning even small amounts can trigger these severe muscular effects.
Wooden Chest Syndrome: When Fentanyl Freezes the Body
Although fentanyl’s muscle-relaxing effects often cause the characteristic bent posture seen in users, the drug can paradoxically trigger the opposite reaction, a condition called wooden chest syndrome (WCS). While fentanyl causes slouching in most cases, WCS produces severe skeletal muscle rigidity that freezes your thoracic and abdominal muscles, making ventilation nearly impossible. Fentanyl’s high lipophilicity allows it to readily cross the blood-brain barrier, enabling rapid interaction with the central nervous system.
WCS occurs when fentanyl binds to µ-opioid receptors, activating dopaminergic pathways in your basal ganglia. This triggers prolonged chest wall contraction rather than relaxation. You’ll experience hypoxia, hypercapnia, and resistance to ventilation without airway obstruction. High doses or rapid administration of fentanyl significantly increase the risk of developing this syndrome.
Treatment requires immediate intervention. Naloxone rapidly reverses the rigidity by blocking opioid receptors. Neuromuscular blocking agents like rocuronium manage severe cases. Cessation of fentanyl typically improves symptoms within one hour.
Why Slowed Breathing Forces the Body to Fold
Beyond these acute muscular effects, fentanyl’s most dangerous action unfolds in your brainstem, where it systematically dismantles the neural circuits controlling each breath. Fentanyl sedation effects activate mu-opioid receptors that inhibit your brain’s respiratory centers, suppressing the central pattern generators coordinating breathing muscles.
Fentanyl’s deadliest mechanism quietly dismantles your brainstem’s breathing circuits, silencing the neural rhythm that keeps you alive.
Your body experiences:
- Rapidly declining respiratory rate and tidal volume within minutes of exposure
- Failed compensatory responses as rising CO2 levels can’t trigger adequate breathing
- Progressive hypoxia starving your brain of oxygen, causing cellular death
- Cyanosis presenting as blue-tinged lips, skin, and nails
This oxygen deprivation compounds postural collapse. Your muscles lose tone, your awareness dims, and your body folds forward, unable to maintain upright positioning as fentanyl’s 70-times-greater-than-morphine potency overwhelms respiratory drive. Making matters worse, naloxone, the standard overdose reversal medication, reverses fentanyl less readily than it reverses morphine, leaving victims trapped in respiratory failure longer. If you witness someone experiencing these symptoms, contacting emergency services and the appropriate resources can help investigate the situation and potentially save a life.
Fentanyl Fold Warning Signs That Signal Overdose
Recognizing fentanyl fold warning signs can mean the difference between life and death when someone’s overdosing. You’ll observe multiple RespiratoryFailureSigns alongside the characteristic bent posture, including slow or absent breathing, gurgling sounds, and choking.
| Warning Sign | Presentation | Timeframe |
|---|---|---|
| Pinpoint pupils | Constricted even in low light | Minutes after exposure |
| Breathing changes | Slow, shallow, or stopped | Within 5 minutes |
| Skin discoloration | Blue/grey lips and nails | Progressive with hypoxia |
| Unresponsiveness | Won’t respond to shaking | Seconds to minutes |
| Body changes | Limp muscles, possible stiffening | Advanced overdose |
You should act immediately if you notice someone folded over displaying these signs. Peak respiratory depression occurs within five minutes, leaving minimal time for intervention. If you suspect an overdose, naloxone can rapidly reverse the effects of opioids and restore normal breathing within 2-3 minutes when administered in time.
How to Respond When You See a Fentanyl Fold
When you spot someone in the fentanyl fold position, you’re likely witnessing active neurological impairment that can progress to fatal respiratory depression within minutes. Your immediate response should follow three critical steps: recognize the overdose warning signs, call 911 without hesitation, and administer naloxone if you have access to it. These actions are time-sensitive because evidence shows 90% of fentanyl overdose decedents are pulseless by the time EMS arrives.
Recognize the Warning Signs
Because fentanyl’s potency exceeds morphine by up to 100 times, recognizing the warning signs of intoxication can mean the difference between life and death. Fentanyl intoxication symptoms manifest through multiple physiological systems simultaneously, progressing rapidly toward respiratory failure.
Watch for these critical indicators:
- Postural collapse: The body folds forward at the waist, unable to maintain upright positioning due to motor control failure.
- Respiratory compromise: Breathing becomes shallow, slow, or absent, often accompanied by choking or gurgling sounds.
- Altered consciousness: The person drifts between wakefulness and unconsciousness, remaining unresponsive to verbal or physical stimuli.
- Physical markers: Pinpoint pupils, cold or clammy skin, and bluish discoloration of lips and fingernails signal oxygen deprivation.
You shouldn’t delay intervention when observing these symptoms, respiratory arrest can occur within minutes.
Call Emergency Services Immediately
The moment you observe someone locked in the characteristic fentanyl fold, that rigid forward bend at the waist with an inability to self-correct, you’re witnessing a medical emergency that demands immediate action. Understanding why fentanyl makes people bend over helps you recognize this posture as a critical warning sign requiring urgent response. Factors influencing fentanyl posture can vary widely, from individual tolerance levels to the specific circumstances of drug use. Each factor plays a vital role in how the body reacts, revealing much about the severity of the situation. Recognizing these influences not only aids in timely intervention but also fosters a deeper understanding of the challenges faced by users.
Dial 911 immediately and provide your exact location. Describe what you’re seeing: a sharp waist bend with a frozen, semi-conscious position. Tell dispatchers you suspect fentanyl overdose. Report additional symptoms like shallow breathing or blue lips.
Why do fentanyl users bend over? The neurological impairment is severe enough that their bodies can’t maintain normal posture. This semi-conscious state can rapidly progress to full respiratory failure. Stay on the line and follow all dispatcher instructions until help arrives.
Administer Naloxone if Available
Naloxone acts as a competitive opioid receptor antagonist that can reverse the life-threatening respiratory depression you’re witnessing in someone displaying the fentanyl fold. You should expect breathing restoration within 2-3 minutes of administration. Due to fentanyl’s potency, you’ll likely need multiple doses, potentially 10 mg total for synthetic opioids.
- Peel the nasal spray package and insert the nozzle until your fingers touch the nostril base
- Press the plunger firmly to deliver the full dose
- Administer a second dose in the alternate nostril if there’s no response within 2-3 minutes
- Continue dosing every 2-5 minutes while monitoring for chest wall rigidity
Monitor the person for 4-12 hours post-administration since naloxone’s half-life (30-80 minutes) is shorter than fentanyl’s duration, risking re-sedation.
How Long Does the Fentanyl Fold Last?
How long the fentanyl fold lasts varies noticeably depending on dose, route of administration, and individual physiology. If you’ve used intravenously, you’ll experience peak effects within minutes, with the fold potentially resolving in 30-60 minutes. Tablets, lozenges, or sprays typically produce effects lasting 4-6 hours.
Your body’s fat tissue plays a critical role. If you’re a chronic user, fentanyl accumulates in fat stores, extending clearance time and prolonging the bent posture. The neuromuscular rigidity affecting trunk muscles can persist for hours after the initial high subsides.
You should expect the fold to resolve gradually, typically within 45 minutes to one hour for some individuals. However, muscle weakness and CNS depression may linger considerably longer. Resolution often occurs upon awakening or when someone provides physical assistance.
When the Fentanyl Fold Becomes a Medical Emergency
While the fentanyl fold itself signals significant CNS depression, certain accompanying signs indicate you’re witnessing a life-threatening emergency requiring immediate intervention.
The fentanyl fold isn’t just concerning, it’s your urgent signal that death may be moments away without intervention. The fentanyl fold isn’t just concerning, it’s an urgent clinical warning that life-threatening respiratory depression may be imminent without rapid intervention. Understanding the risks and benefits of fentanyl fold helps clinicians and bystanders recognize this red flag early and respond quickly to prevent fatal outcomes.
You must act immediately when observing these critical warning signs:
- Respiratory failure markers: Breathing falls below 8 breaths per minute, or you notice gurgling sounds indicating airway obstruction
- Hypoxia indicators: Lips, fingertips, or nail beds turn blue or gray, signaling dangerously low oxygen saturation
- Unresponsiveness: The person doesn’t react to loud voice commands or sternal rub stimulation
- Wooden chest syndrome: Torso rigidity prevents adequate lung expansion, rapidly accelerating oxygen depletion
Call emergency services immediately and administer naloxone if available. Fentanyl’s potency means the window between the fold and fatal respiratory arrest narrows quickly, minutes determine survival outcomes.
Breaking free from the fentanyl fold is possible with the right support. At Villa Treatment Center, our experienced team in Woodland Hills provides personalized, evidence-based treatment plans tailored to your needs. From medically supervised detox and intensive drug addiction treatment, to residential rehabilitation and flexible outpatient care, we stand by your side at every step. A life free from fentanyl dependence is within your reach. Call +1 (818) 639-7160 today and begin your journey toward healing.
Frequently Asked Questions
Can Someone Experiencing the Fentanyl Fold Still Hear or Understand You?
You likely can’t rely on someone in the fentanyl fold to hear or understand you. Severe central nervous system depression slows brain activity controlling alertness, which impairs their ability to process external stimuli. They may appear semi-conscious or completely unresponsive, with confusion and disorientation blocking comprehension of verbal input. If they’re not responding to your voice or touch, this signals a potentially life-threatening state requiring immediate naloxone intervention.
Does Naloxone Reverse the Fentanyl Fold Immediately After Administration?
Naloxone doesn’t reverse the fentanyl fold immediately. When you administer intranasal naloxone, it reaches peak plasma concentration after approximately 15 minutes, though you may see initial reversal signs within 2-3 minutes. The bent posture results from opioid-induced muscle relaxation and neurological suppression, which resolve as naloxone displaces fentanyl from mu-opioid receptors. You should administer a second dose if you don’t observe improvement within three minutes.
Why Do Some Fentanyl Users Remain Standing While Bent Over?
You’ll notice some users remain standing because fentanyl doesn’t completely eliminate all muscle function, it selectively impairs postural control while leaving enough residual muscle tone to prevent total collapse. Your brain’s motor signals become severely compromised, but antigravity muscles in the legs may retain partial function. You’re fundamentally caught between consciousness and unconsciousness, where your body can’t correct its position but maintains just enough strength to avoid falling completely.
Can the Fentanyl Fold Occur From Prescription Fentanyl Patches?
Yes, you can experience the fentanyl fold from prescription patches, though it’s less common than with illicit fentanyl. You’re most at risk if you misuse patches, chewing them, extracting the gel for injection, or applying multiple patches simultaneously. Combining patches with alcohol or benzodiazepines also increases your likelihood of developing this dangerous posture. The fold signals significant CNS depression regardless of fentanyl’s source; potency drives the effect, not origin.
Does Body Weight or Tolerance Affect How Severe the Fold Appears?
Your body weight doesn’t greatly/markedly/appreciably affect how severe the fold appears, as fentanyl-induced muscle rigidity occurs regardless of weight variations. However, your tolerance level does influence duration rather than severity, if you’re a long-term user, drug accumulation in fat tissue delays clearance, potentially keeping you bent for over an hour. The fold’s intensity stems primarily from trunk muscle rigidity and CNS depression, not weight-related factors.